Virus vs Flu vs Cold: The Real Differences Your Doctor Wants You to Know
You wake up with a scratchy throat, and your first thought is: “Great. Is this a cold, the flu, or something worse?” Most people guess wrong — then treat it wrong, feel worse longer, and wonder why their “cold” lasted three weeks. This guide changes how you think about every future illness you or your family catches.
What Actually Causes a Cold, Flu, or “Viral Illness”
Before we compare symptoms, let’s get the biology straight — because it changes everything about how you respond.
A “virus” is not a diagnosis. It is a category. Over 200 different viruses cause what we casually call a cold. Rhinovirus is the most common culprit, responsible for roughly 50% of cold cases, but adenoviruses, coronaviruses unrelated to COVID-19, and RSV also trigger cold-like symptoms. When your doctor says, “it’s just a viral illness,” they’re telling you antibiotics won’t help — not that all viruses are equal.
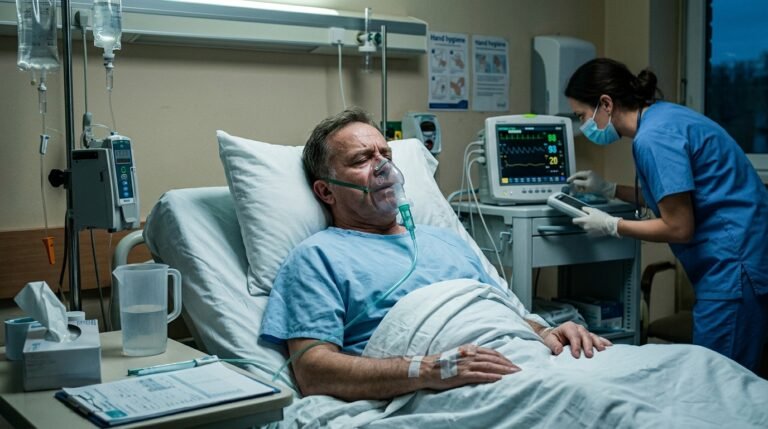
Influenza is specific. The flu comes from influenza A or influenza B viruses. These are different animals entirely. They hijack your cells more aggressively, replicate faster, and trigger a far more intense immune response than a typical cold virus. That’s why the flu makes you feel like you were hit by a truck, while a cold makes you feel like you’ve annoyed someone.
The Symptom-by-Symptom Breakdown
This is where most articles fail you. They drop a vague table and call it done. Let’s be more useful.
Onset is your first and most powerful clue. Colds creep in. A tickle. A sneeze. Then mild congestion builds over 24 to 48 hours. Flu does not creep anywhere — it hits you in the middle of a Tuesday afternoon, and within two hours, you are lying on your couch, wondering if you will survive the night (you will). That abruptness is almost diagnostic by itself.
Fever tells the next chapter. True colds rarely produce significant fever in adults — if present at all, it’s usually below 101°F and brief. Flu fever is real: 101°F to 104°F, lasting three to four days, with cycling chills and sweats. If you’re drenched in sweat while shivering at 102°F, that is almost certainly the flu.
Body aches flip the discomfort scale entirely. With a cold, you feel slightly run-down. With flu, your muscles ache with a kind of violence — patients often describe it as “worked out for six hours, then got punched.” That’s the cytokine storm doing its work, not the virus itself.
Respiratory symptoms favor the cold. Runny nose, congestion, and sneezing are cold hallmarks. Flu usually starts with a dry cough and chest tightness, while nasal symptoms are secondary. If your nose is the main event and you have minimal fever, you’re dealing with a cold.
| Symptom | Cold | Flu |
|---|---|---|
| Onset speed | Gradual (1–2 days) | Sudden (hours) |
| Fever | Runny/stuffy nose | Common, 101–104°F |
| Body aches | Mild | Severe |
| Headache | Uncommon | Common, throbbing |
| Fatigue | Mild | Severe, sudden |
| Runny / stuffy nose | Very common | Sometimes |
| Sneezing | Common | Occasional |
| Sore throat | Common | Sometimes |
| Chest discomfort | Mild or none | Often present |
| Duration | 7–10 days | 5–7 days (weakness lingers 2+ weeks) |
The 48-Hour Window That Changes Your Treatment Plan
Here is something most articles skip over entirely: antiviral medications like oseltamivir (Tamiflu) are only effective when taken within the first 48 hours of flu symptom onset. After that window closes, they provide minimal benefit. This makes knowing whether you have flu — not just “a virus” — a genuine clinical question with real consequences.
If you’re in a high-risk group (over 65, pregnant, immunocompromised, or have chronic heart or lung disease), getting a rapid flu test within the first day of symptoms is worth an urgent care visit.
Colds have no antiviral treatment. The average cold clears in 7 to 10 days, with symptoms peaking at days 2 to 3. If you’re still congested at day 10 with worsening facial pain, consider whether you’ve developed a secondary bacterial sinus infection — a separate issue needing a different approach.
Why Your Immune System Responds So Differently
When rhinovirus enters your nasal passages, your immune system mounts a localized response. The runny nose and congestion are largely your own immune system’s doing — mucus intentionally trapping and flushing the virus out. You are feeling your body work.
Influenza is more invasive. It binds to receptors deep in your airways and replicates with remarkable speed. The fever, muscle aches, and crushing fatigue you feel are caused by your immune system releasing interferons and cytokines body-wide. That’s why flu feels like a whole-body event — not just a nose event.
This also explains something counterintuitive: healthy adults in their 20s and 30s can have the hardest time with the flu. A strong, reactive immune system produces a more intense cytokine response — more severe symptoms. Older adults may feel less acutely terrible but face higher risks of serious complications like pneumonia.
What Actually Works for Relief (And What Is a Waste of Money)
Let’s be direct. Most cold remedies on pharmacy shelves offer minimal evidence-based benefit.
Zinc lozenges have the best evidence for shortening cold duration — but only when started within 24 hours of the first symptom. Research suggests a reduction of about one day. Not dramatic, but real. Brands like Zicam and Cold-Eeze use zinc acetate or zinc gluconate. Zinc sulfate doesn’t absorb the same way — check the label.
Vitamin C does almost nothing for treatment once you’re already sick, despite worldwide grandmother consensus. It shows modest benefit only for extremely deficient people or those under intense physical stress, like endurance athletes.
Honey for cough — actually works. A study published in Pediatrics found dark buckwheat honey more effective than dextromethorphan (a common OTC cough suppressant) in children aged 2 to 18. A tablespoon at bedtime is cheap, pleasant, and genuinely useful.
Saline nasal rinses (NeilMed, neti pots) reduce congestion and help clear viral particles from the nasal passages. This is probably the most underrated tool on this list — the evidence is solid, and the cost is almost nothing.
For flu: rest and hydration are the treatment. The Tamiflu window is critical. Beyond that, acetaminophen or ibuprofen handles fever and aches effectively.
The Flu Shot: Honest Assessment
The flu vaccine does not prevent all cases of flu. In a good match year, effectiveness reaches 60–70% in healthy adults. In a poor match year, around 40–50%. Still meaningful — especially for reducing severe outcomes.
The argument most people don’t hear: even when the vaccine doesn’t prevent infection, it significantly reduces the severity of illness and risk of complications like pneumonia or hospitalization. For people over 65, children under 5, pregnant women, and anyone with a chronic condition, the flu vaccine is among the most cost-effective health interventions available.
The flu shot cannot give you the flu. The injected vaccine contains inactivated virus particles that cannot replicate. If you felt sick after your shot, you caught something else around the same time — or had a mild immune response to the vaccine itself, which is a sign it is working.
When to Stop Self-Treating and Go to the Doctor
Most healthy adults can manage colds and uncomplicated flu at home. But certain signs demand immediate medical attention, regardless of what you think you have.
Go to urgent care or the ER immediately if you have:
- Difficulty breathing or shortness of breath at rest
- Persistent chest pain or pressure
- Severe vomiting that prevents staying hydrated
- Confusion, disorientation, or unusual behavior
- Symptoms that improve, then suddenly worsen significantly
- Bluish or grayish color around the lips or fingernails
- In children: unusual lethargy, fast breathing, or no wet diapers for 8 hours
For high-risk individuals — adults over 65, pregnant women, people with asthma, diabetes, or heart disease — the threshold for seeking care should be lower. A flu that knocks a healthy 30-year-old out for a week can put a 70-year-old in serious trouble.
COVID-19: How It Fits Into the Picture
COVID-19 shares significant symptom overlap with both cold and flu, which is one of its most frustrating characteristics. Fever, body aches, fatigue, and respiratory symptoms appear in all three.
The honest answer: you cannot reliably distinguish COVID-19, flu, and severe cold by symptoms alone in many cases. If isolation, treatment, or protecting vulnerable people matters, a rapid test is the only way to know. Rapid antigen tests for both COVID-19 and flu are widely available and give results in 15 minutes.
Frequently Asked Questions
Can you have the flu without a fever?
Yes, and more commonly than people assume — especially in adults who take fever-reducing medications early, or in older adults whose baseline temperature runs lower. Don’t use the absence of fever as your sole reason to dismiss flu.
Is it possible to have a cold and the flu at the same time?
Technically, yes, though uncommon. Both viruses can infect you simultaneously, typically resulting in more severe illness. If you feel worse than a typical cold but your rapid flu test came back negative, retest at 24 to 48 hours — early tests can produce false negatives.
Why do I always get sick in winter?
Cold, dry air dries out nasal mucous membranes, reducing their ability to trap viruses. People spend more time indoors in close contact. Influenza viruses survive and transmit more efficiently in cold, dry conditions. Winter conditions make transmission easier — cold weather itself doesn’t cause illness, viruses do.
Should I exercise when I’m sick?
A rough guide: if symptoms are above the neck with no fever, light exercise may be fine. If you have fever, body aches, chest symptoms, or severe fatigue, rest completely. Exercising during flu stresses your cardiovascular system and, in rare cases, has been linked to myocarditis.
How long am I contagious with the flu?
From about one day before symptoms start until five to seven days after onset. Children and immunocompromised individuals may be contagious longer. This pre-symptomatic window is why flu spreads so efficiently — you’re sharing it before you know you have it.
What is the fastest way to recover from a cold?
Rest, hydration, zinc lozenges started within 24 hours of symptoms, saline nasal rinses, and honey for cough. There is no magic pill. Your immune system does the work — your job is to stop getting in its way by staying up late, skipping fluids, and trying to power through when your body is asking you to stop.
The Bottom Line
Cold: Gradual onset, nose-dominated, manageable at home, clears in a week.
Flu: sudden and severe, full-body symptoms, high fever. Rest and antivirals within 48 hours matter.
Other viral illnesses. Use your judgment, test when it matters to you or to vulnerable people around you, and know your red flags.
The single best change you can make starting today: get comfortable with at-home rapid testing so you always know what you’re dealing with, and treating flu like a cold means missing your treatment window. Treating a cold like the flu means unnecessary medical visits and wasted money.