What Is the Difference Between Flu A and Flu B? The Complete Guide
Flu A and Flu B are both influenza viruses, but they are not the same illness. Flu A is more severe, drives every major flu pandemic, and mutates faster. Flu B is milder on average but causes a disproportionate share of child deaths. Both respond to the same antivirals — if you act within 48 hours.
This guide covers the key differences in symptoms, severity, duration, treatment, and risk so you know exactly what you are dealing with and what to do next.

What Are Influenza A and Influenza B, Exactly?
Let us start with the biology, because it genuinely changes how you think about your treatment options.
Both Flu A and Flu B are RNA viruses in the Orthomyxoviridae family. They hijack your respiratory cells, replicate explosively, and trigger the full-body immune response you experience as fever, fatigue, and body aches. But they are not the same organism.
Flu A: The Shape-Shifter
Influenza A infects humans, birds, pigs, horses, seals, and other animals. That cross-species range is exactly why Flu A is responsible for every major flu pandemic in recorded history, including the 1918 Spanish Flu (H1N1), the 2009 swine flu outbreak, and every significant global health scare in between.
Flu A viruses are classified by two surface proteins: hemagglutinin (H) and neuraminidase (N). There are 18 known H subtypes and 11 known N subtypes. The strains circulating most commonly in humans right now are H1N1 and H3N2. H3N2 seasons tend to produce the highest hospitalization and death rates, particularly in adults over 65.
The virus mutates so rapidly through a process called antigenic drift that last year’s vaccine may provide only partial protection this year. Pandemic-level change happens through antigenic shift, when two different flu A strains infect the same host simultaneously and swap genetic material.
Flu B: The Human Specialist
Influenza B infects almost exclusively humans (and, rarely, seals). Because it does not jump between species the way Flu A does, it lacks the pandemic potential of its counterpart. It also mutates more slowly.
Flu B divides into two distinct lineages: B/Yamagata and B/Victoria. For years, predicting which lineage would dominate the season was a genuine public health guessing game. As of the 2024-2025 season, B/Yamagata appears to have been eliminated globally, making B/Victoria the only circulating Flu B lineage. That is a significant development that most mainstream flu articles have not yet caught up with.
Flu B tends to circulate later in flu season, often peaking in February and March when Flu A activity starts declining. So if you get hit in late winter, there is a real chance you are dealing with Flu B rather than Flu A.
Flu A vs. Flu B: Side-by-Side Comparison
Here is a practical comparison of the two strains across the factors that matter most to patients and families.
| Factor | Influenza A | Influenza B |
| Hosts | Humans, birds, pigs, horses, and more | Primarily humans (rarely seals) |
| Pandemic risk | High — responsible for all major flu pandemics | Very low — no pandemic potential |
| Severity | Generally more severe, esp. H3N2 strains | Milder on average, but hospitalizations occur |
| Mutation rate | Very fast (antigenic drift and shift) | Slower, more stable genetically |
| Peak timing | Earlier in flu season (Nov-Jan typically) | Later in flu season (Feb-Mar typically) |
| Common subtypes | H1N1, H3N2 | B/Victoria lineage (as of 2024-2025) |
| Treatment | Oseltamivir, baloxavir, peramivir | Same antivirals — same efficacy |
| Children | Severe in young children | Disproportionately affects children |
Are the Symptoms of Flu A and Flu B Different?
This is the question I get asked most often, and the honest answer is: not in any way you can reliably tell without a test.
The clinical presentation of Influenza A and Influenza B overlaps almost completely. Both cause sudden-onset fever (typically 100-104 F), severe body aches, headache, fatigue, dry cough, and sore throat. Both can cause chills, nasal congestion, and, particularly in children, vomiting and diarrhea.
Where Subtle Differences Appear
Some research suggests Flu B may cause more pronounced gastrointestinal symptoms, including nausea and abdominal pain, than Flu A. A 2019 study in the Journal of Infectious Diseases found slightly higher rates of myositis (severe muscle inflammation) in children with Flu B infections.
But here is the real-world problem: you cannot self-diagnose which flu you have based on symptoms alone. The rapid influenza diagnostic tests (RIDTs) available at urgent care clinics, and the more accurate PCR-based molecular assays, are the only reliable way to distinguish between strains. If you are sick enough to be wondering which flu you have, you are sick enough to get tested.
One practical tip from a nurse practitioner I spoke with: ‘If your kid has a high fever AND is complaining that their legs hurt badly, that muscle pain pattern sometimes points toward Flu B. But we still run the test every time. Guessing costs people valuable treatment windows.’
Which Is More Dangerous: Flu A or Flu B?
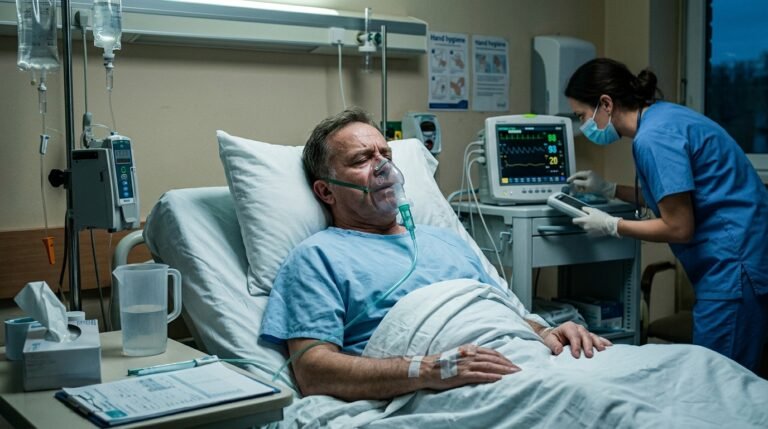
Flu A kills more people annually. That is the bottom line. CDC data from the last decade consistently shows that Flu A H3N2 seasons produce the highest all-cause excess mortality, with adults 65 and older bearing the greatest burden.
The 2017-2018 flu season, which was H3N2-dominant, is estimated to have killed 52,000 Americans and caused 710,000 hospitalizations. It was one of the deadliest flu seasons in recent decades. Flu B-dominant seasons do not produce numbers like that.
Where Flu B Punches Above Its Weight
Flu B is not benign for everyone. Several well-documented patterns show it can be especially dangerous in specific groups.
Children under 5: Multiple studies have shown that Flu B causes a disproportionately high share of pediatric flu deaths. A CDC analysis covering ten flu seasons found Flu B accounted for 40% of pediatric deaths despite representing a smaller share of overall infections.
Reye’s syndrome risk: This rare but life-threatening condition, which causes swelling in the brain and liver, has been most commonly associated with Flu B infection in children who receive aspirin. Never give aspirin to children with flu symptoms.
Myositis and rhabdomyolysis: Flu B appears slightly more likely than Flu A to cause severe muscle breakdown in children, sometimes requiring hospitalization for kidney protection.
Important: If a child with flu symptoms cannot walk, is extremely lethargic, or has severe leg pain, seek emergency care immediately. These can be signs of flu-associated myositis, more common with Flu B.
How Long Does Flu A Last Compared to Flu B?
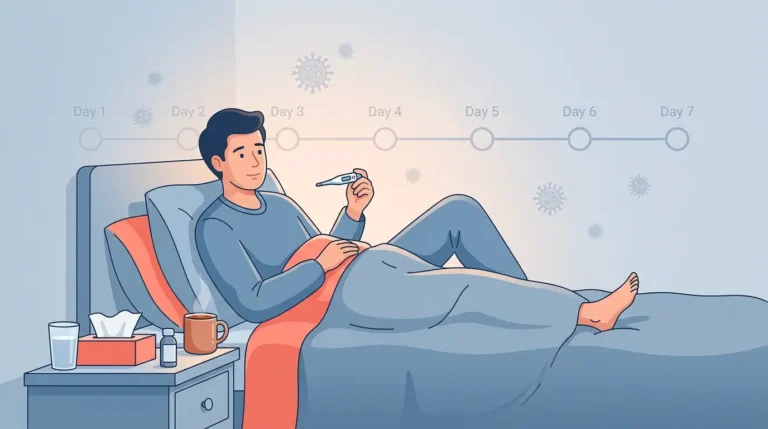
Both strains typically run a similar course in otherwise healthy adults. Expect the worst of the fever and body aches to peak within 24-48 hours of symptom onset, with acute illness lasting 5-7 days in most uncomplicated cases.
Fatigue and cough, however, can linger for 2-3 weeks after the fever resolves. This post-viral exhaustion catches a lot of people off guard. They feel almost human on day 7, go back to full activity on day 8, and wonder why they crash on day 9.
Factors That Extend Illness Duration
- Age over 65 or under 5
- Underlying conditions: asthma, COPD, diabetes, heart disease
- Immunocompromised status from cancer treatment, HIV, or transplant medications
- Delayed antiviral treatment (beyond 48 hours of symptom onset)
- Secondary bacterial pneumonia, which can extend acute illness by weeks
Flu A H3N2, in particular, tends to produce longer and more severe illness in older adults than B strains. If you are 65+ and testing positive for H3N2, your doctor should have a low threshold for antiviral prescribing and follow-up monitoring.
How Is Flu A vs. Flu B Diagnosed?
This matters more than most people realize, because treatment decisions hinge on it.
Your options for testing range from fast-but-less-accurate to slower-but-definitive.
Rapid Influenza Diagnostic Tests (RIDTs)
These are the most common tests used in urgent care and doctor’s offices. Results come back in 15-30 minutes. The problem is sensitivity: RIDTs miss anywhere from 40-70% of actual flu infections, meaning a negative result does not rule out flu. Specificity is high, so a positive is usually trustworthy, but a negative during peak flu season should prompt your doctor to treat based on symptoms anyway.
Standard RIDTs will tell you if influenza is present and whether it is Type A or Type B. They do not identify the specific subtype (H1N1 vs. H3N2).
Molecular Assays (PCR-Based Tests)
PCR-based flu tests are significantly more accurate, with sensitivity above 90% in most studies. Many hospital labs and some urgent care centers now use these. They take longer (1-8 hours depending on the platform), but they can identify influenza A subtypes and distinguish Flu B lineages. If you are hospitalized with flu-like illness, this is the test you want.
At-home rapid flu tests entered the consumer market in force during 2023-2024. The Lucira Health flu test and similar products offer PCR-level accuracy at home, with results in 30 minutes. These are worth having if you are immunocompromised or care for vulnerable family members.
What Is the Best Treatment for Flu A and Flu B?
The treatment approach for both Flu A and Flu B is essentially the same, which is one piece of genuinely good news. Antivirals approved by the FDA work against both types.
Antiviral Medications
Oseltamivir (Tamiflu): The most widely used antiviral. Works for both Flu A and Flu B. Must be started within 48 hours of symptom onset for maximum benefit. Reduces illness duration by approximately 1-1.5 days and significantly cuts hospitalization risk in high-risk patients. Available as capsules and liquid. Generic versions are widely available and cost around $30-80 depending on insurance status as of early 2025.
Baloxavir marboxil (Xofluza): A single-dose oral antiviral approved in 2018. Effective against both Flu A and Flu B, including some oseltamivir-resistant strains. Works via a different mechanism, inhibiting the viral polymerase rather than neuraminidase. Priced at approximately $150-200 without insurance, though manufacturer coupons reduce this significantly.
Zanamivir (Relenza): An inhaled antiviral that works well for both strains but is not recommended for people with respiratory conditions like asthma, due to bronchospasm risk.
Peramivir (Rapivab): An IV antiviral used in hospitalized patients who cannot take oral medications.
The 48-Hour Window: Why It Is Non-Negotiable
Every antiviral guideline stresses the 48-hour window for good reason. A 2021 meta-analysis in The Lancet found that oseltamivir started within 12 hours of symptom onset reduced hospitalization risk by 63% compared to no treatment. That benefit drops substantially after 48 hours, though antivirals may still reduce severity even when started later in high-risk patients.
The practical implication: if you are in a high-risk group (over 65, under 5, pregnant, immunocompromised, or have chronic conditions), do not wait to ‘see how it goes.’ Get tested and treated within the first day of symptoms.
Flu Genie Reminder: Antiviral treatment within 48 hours is the single most impactful action you can take after a positive flu diagnosis. If your provider hesitates to prescribe, ask specifically about your risk profile.
Does the Flu Shot Protect Against Both Flu A and Flu B?
Yes, with an important asterisk.
Standard quadrivalent flu vaccines contain four components: two Flu A strains (H1N1 and H3N2) and two Flu B strains (one B/Victoria and one B/Yamagata). Since B/Yamagata now appears to have been globally eradicated, the 2025-2026 vaccine formulations are expected to shift to trivalent coverage, removing the B/Yamagata component.
Vaccine effectiveness varies considerably by season. In years when the vaccine strains match the circulating viruses well, effectiveness against symptomatic flu ranges from 40-60%. In mismatched years (particularly against H3N2, which mutates rapidly), effectiveness can drop to 20-30%.
High-Dose and Adjuvanted Vaccines for Older Adults
Adults 65 and older should specifically ask for Fluzone High-Dose Quadrivalent or FLUAD Quadrivalent (adjuvanted). These formulations consistently outperform standard-dose vaccines in this age group, with one meta-analysis showing a 24% relative reduction in flu-related hospitalization compared to standard doses.
Who Is Most at Risk From Flu A and Flu B?
Understanding your personal risk profile changes how aggressively you should pursue testing and treatment.
High-Risk Groups for Flu A
- Adults 65 and older, particularly during H3N2-dominant seasons
- People with chronic cardiovascular disease — flu doubles heart attack risk in the days following infection
- Pregnant women, who face elevated risk of severe complications in all trimesters
- People with chronic pulmonary disease, including asthma and COPD
High-Risk Groups for Flu B
- Children under 16, particularly under 5, who show disproportionate severity
- Children on chronic aspirin therapy (Reye’s syndrome risk)
- Individuals with neuromuscular conditions, increasing aspiration pneumonia risk
- Adolescents, who some research suggests are more susceptible to B/Victoria lineage specifically
Can You Have Flu A and Flu B at the Same Time?
Technically yes, though co-infection is rare. Simultaneous infection with both influenza A and B has been documented in case reports, and dual-infection rates reportedly increased during the 2020-2021 pandemic period when masking and social distancing suppressed flu transmission, then relaxed.
During the 2022-2023 flu season, several US hospitals reported small clusters of co-infections, particularly in immunocompromised patients. PCR-based molecular testing can identify both strains simultaneously, while rapid antigen tests may only flag one.
If your symptoms are unusually prolonged or biphasic (you start improving, then get significantly worse), mention the possibility of co-infection to your provider. It is rare but does exist and changes the clinical picture.
Flu A vs. Flu B in Children: What Parents Need to Know
If I am being completely direct, Flu B deserves more parental respect than it typically gets. The cultural shorthand of ‘Flu B is the milder one’ has real consequences when parents delay treatment.
A large retrospective study of pediatric flu deaths over ten flu seasons found that Flu B caused 40% of child flu deaths despite accounting for a smaller proportion of total flu cases. The case fatality rate for Flu B in children was actually higher than for Flu A in some age brackets.
Warning Signs in Children That Require Immediate Medical Attention
- Difficulty breathing or fast, labored breathing
- Bluish lips or face (sign of oxygen deprivation)
- Severe or unrelenting vomiting that prevents fluids
- Child is unresponsive or cannot be woken
- Severe leg pain or refusal to walk (possible myositis)
- Symptoms improve and then return with fever and worsening cough
The last point on that list, a pattern of apparent improvement followed by sudden deterioration, is a classic sign of secondary bacterial pneumonia, which can follow both Flu A and Flu B infection.
Never give aspirin to a child or teenager with flu symptoms. Aspirin use during influenza infection is associated with Reye’s syndrome, a rare but potentially fatal condition causing brain and liver damage. Use acetaminophen or ibuprofen instead.
The Bottom Line: Flu A vs. Flu B
The difference between Flu A and Flu B is not academic. Flu A is more severe on average, responsible for all major pandemics, and more common earlier in flu season. Flu B is often underestimated, especially in children, where it punches well above its weight in terms of hospitalizations and deaths.
Both strains respond to the same antivirals. Both can make a healthy adult genuinely miserable for a week. And both are best treated within 48 hours of symptom onset for maximum benefit.
The three actions most likely to change your outcome: get your flu shot before October, get tested at the first sign of symptoms if you are in a high-risk group, and take antiviral treatment seriously rather than toughing it out.
If you have ever sat in an urgent care waiting room at 2 a.m. wondering which letter your child’s fever belongs to, now you know exactly what that distinction means and what to do about it.
Frequently Asked Questions About Flu A vs. Flu B
Is Flu A contagious longer than Flu B?
Both strains have similar contagious periods. You are most contagious during the 24 hours before symptoms appear and for 5-7 days after illness begins. Immunocompromised individuals may shed virus for considerably longer, sometimes weeks, regardless of strain.
Does Flu B ever cause pandemics?
No. Flu B infects only humans and lacks the genetic mechanisms needed for pandemic-scale emergence. All historical and modern flu pandemics have been caused by Influenza A strains that acquired new genes from animal reservoirs. This is one genuinely reassuring aspect of a Flu B diagnosis.
Why does H3N2 cause more severe illness than other flu strains?
H3N2 has a particularly strong ability to evade immune responses, mutates rapidly, and preferentially infects the upper and lower respiratory tract with high efficiency. It also tends to cause more severe illness in older adults because their immune memory from earlier exposure to related strains offers less protection than expected.
Can I get Flu A and Flu B in the same flu season?
Yes, and it happens more often than people expect. If you had Flu A in November and recover fully, you remain susceptible to Flu B when it peaks in February or March. Flu shot or not, recovery from one type does not protect you against the other.
How do I know if I need Tamiflu for Flu B specifically?
The same clinical criteria apply for both strains. You should strongly consider antiviral treatment if you are in a high-risk group (over 65, under 5, pregnant, immunocompromised, or have chronic conditions), if you are sick enough to consider hospitalization, or if you start treatment within 48 hours of symptom onset. For otherwise healthy adults with mild symptoms, the benefit is modest but real.
Is Flu B less common than Flu A?
Generally yes. In most flu seasons, Flu A accounts for the majority of circulating influenza viruses, particularly early in the season. Flu B typically makes up 15-40% of flu cases depending on the year, with some seasons seeing near-equal co-circulation. The CDC FluView tracker provides real-time season data.
Can animals give me Flu B?
Essentially no. Unlike Flu A, which can be transmitted from birds, pigs, and other animals to humans, Flu B is almost exclusively a human virus. The rare Flu B infections documented in seals have never resulted in human transmission from animals. Your pet cannot give you Flu B.