Can You Get the Flu Back to Back? What Really Happens When the Flu Hits Twice
Yes — you can get the flu back-to-back, and it happens more often than most people realize. The influenza virus is not a single bug. It is a family of constantly changing strains, and catching one strain does not protect you from the others.
According to the CDC, multiple influenza strains — including Influenza A and Influenza B — circulate at the same time every flu season. Your immune system builds defenses against the exact strain it fought. It does not build a shield against every version of the virus.
On top of that, your natural immunity fades over weeks and months. That combination — multiple strains plus shrinking protection — is why some people end up sick twice in the same winter.
This guide covers all of it. By the end, you’ll understand exactly why back-to-back flu is possible, who is most at risk, what your immune system is actually doing during those weeks, and what you can do right now to avoid repeating the experience.

Can You Actually Get the Flu Twice in the Same Season?
Yes — and it happens more often than most people realize. During a typical flu season, two or three strains of influenza circulate simultaneously: usually influenza A (H1N1 and H3N2) and influenza B. Your immune response to one strain provides almost zero cross-protection against the others. So if you catch H1N1 in December and H3N2 rolls through your office in February, your immune system has to fight from scratch.
The CDC tracks this every year, and in most seasons, both influenza A and B are co-circulating by late January. According to surveillance data published in MMWR (Morbidity and Mortality Weekly Report), dual-strain seasons are not rare exceptions — they are the norm. In the 2019–2020 season, for example, influenza B dominated early while influenza A surged in the back half of the season. Millions of people were exposed to both.
Here’s the piece that trips people up: the flu shot is not a one-and-done immunity shield within a season. The quadrivalent vaccine protects against four strains — two A strains and two B strains — but vaccine effectiveness ranges from around 40% to 60% in most years, depending on how well the formulation matches the circulating viruses. That leaves a real gap.
I’ll be direct: if you’ve had the flu once and you feel like you’re invincible for the rest of the season, you are operating on a dangerous myth. The virus doesn’t care about your suffering history.
How Long After the Flu Are You Still Vulnerable?
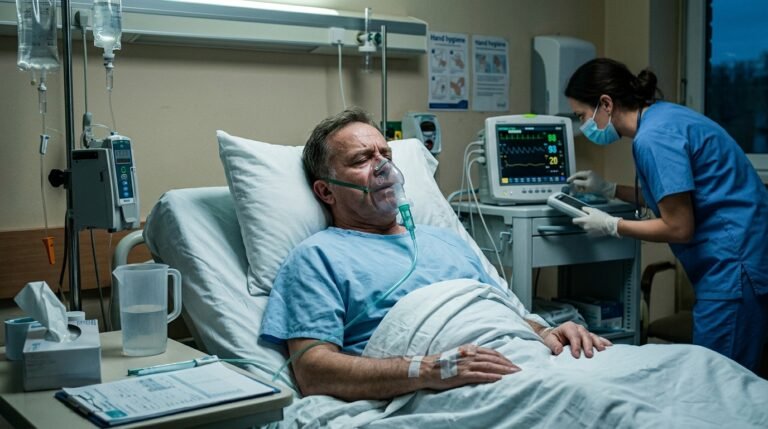
Your immune system is weakest in the two to four weeks immediately following a flu infection. This is the window when back-to-back illness is most dangerous and most likely. Here is what your body is going through during that period.
When influenza infects your respiratory tract, your immune system mounts a response that involves a massive release of cytokines — inflammatory signaling proteins. That cytokine storm is responsible for the body aches, fever, and crushing fatigue you feel. It is also temporarily suppressive to certain immune functions. Think of it like a fire department responding to a five-alarm blaze: every resource is deployed to the current crisis, which leaves other parts of town temporarily unprotected.
A 2020 study published in Nature Immunology found that acute viral infections can induce a state of “trained innate immunity” but also cause temporary depletion of NK (natural killer) cells and cytotoxic T cells that would normally knock out a second invader quickly. In plain language: your immune system is exhausted. And an exhausted immune system is a vulnerable one.
The Two-Week Dead Zone
In the medical community, we informally call the period from day 7 to day 21 post-flu the “recovery window.” You feel better. Your fever is gone. You’re back at work. But your mucosal immunity — the protective layer in your nasal passages and throat that catches viruses before they can establish a foothold — hasn’t fully regenerated. The influenza virus stripped it away. It takes three to four weeks to fully restore.
This is exactly why Sarah got hit twice. She went back to the office on day 10, feeling “mostly fine,” and spent two days commuting on the subway. She had no idea her first line of defense was still down.
What’s the Difference Between Getting the Same Flu Twice vs. a Different Strain?
Getting the exact same flu strain twice in one season is extremely rare but not impossible. Getting two different strains back-to-back is genuinely common. Understanding this distinction matters because it changes how you protect yourself.
When you recover from influenza A (H3N2), your immune system produces strain-specific antibodies. These antibodies recognize the hemagglutinin (H) and neuraminidase (N) proteins on the surface of that specific virus. They are very good at their job against that exact strain. Against influenza B/Victoria or influenza A (H1N1), they offer almost no protection. The surface proteins are too different.
The terminology here matters. When people say they got the “flu” twice, they often mean they had two different respiratory illnesses. Not all of them are influenza. Some may be RSV, rhinovirus, or adenovirus, which your doctor may loosely call the “flu” in conversation. True back-to-back influenza, confirmed by rapid antigen test or PCR, is less common but does happen, especially during dual-strain seasons.
My strong opinion: if you get sick twice in the same season and both illnesses feel flu-like, test for both. Rapid flu tests are available at CVS, Walgreens, and Rite Aid for around $30 as of 2025. Knowing which strain you have changes the antiviral options available to you.
Who Is Most at Risk for Getting the Flu Back-to-Back?
Certain groups face a significantly higher risk of back-to-back influenza. This isn’t about weakness. It’s about immune system biology, exposure levels, and underlying conditions that change how the body responds to infection.
| Risk Group | Why Higher Risk | Key Protection Step |
| Adults 65+ | Immunosenescence slows antibody production | Annual flu shot + Shingrix consultation |
| Children under 5 | Immune system still maturing; high exposure in daycare/school | Full vaccine series; strict sick-day policies |
| Immunocompromised adults | HIV, cancer treatment, organ transplant reduce immune response | HIV, cancer treatment, and organ transplant reduce immune response |
| Healthcare workers | Daily exposure to multiple strains across patient populations | Discuss prophylactic antivirals with the doctor |
| Pregnant women | Immune modulation changes vulnerability and severity | Flu shot recommended in any trimester |
| Frequent flyers/commuters | High-density exposure environments across geographic areas | Mask during peak flu weeks, avoid face-touching |
I’ll share something most articles won’t: healthcare workers I know personally often get hit twice in bad seasons, not because they’re careless, but because their exposure volume is simply too high for any single immune response to compensate for. The biology doesn’t bend to willpower.
Can the Flu Shot Prevent Back-to-Back Flu?
Yes — and it remains your best tool, even though it isn’t perfect. The current quadrivalent flu vaccines (Fluzone, Flucelvax, Fluarix, and others) target four strains simultaneously. Getting vaccinated reduces your risk of any one of those strains and, critically, reduces your risk of severe illness if you do catch a circulating variant.
Here’s my honest take on the flu shot: its effectiveness varies year to year based on how accurately the WHO predicted which strains would dominate when they formulated the vaccine the prior spring. In a good match year (like 2010–2011), effectiveness can reach 60%. In a bad match year (like 2014–2015), it can drop below 20% for H3N2. That variability frustrates people. I understand the frustration.
But here’s what doesn’t change: even a poorly matched vaccine reduces the risk of influenza-related hospitalization by 40% or more in most studies. That’s not nothing. That’s a lot. And for back-to-back flu specifically, a vaccinated immune system tends to recover faster from a first infection, which shortens the vulnerability window for a second one.
High-Dose Vaccine for Adults 65 and Over
Adults 65 and older should specifically ask for Fluzone High-Dose Quadrivalent or Fluad Quadrivalent (adjuvanted). Both contain either four times the antigen or an immune-boosting adjuvant, specifically designed to compensate for immunosenescence. Multiple randomized controlled trials show that these outperform standard-dose vaccines in older adults. As of 2025, they’re covered by Medicare Part B with no copay.
What Are the Symptoms of Getting the Flu a Second Time?
Second-round flu often hits harder than the first, particularly in the weeks immediately following recovery. This surprises people, but it makes sense immunologically. Your body’s resources are still rebuilding. Your mucosal barriers are weakened. You may also be less vigilant about rest and exposure, because you assume you’ve “paid your dues.”
The classic influenza presentation — sudden onset, high fever (102–104°F), severe body aches, dry cough, profound fatigue, and headache — is your key distinguishing feature from a common cold. Colds come on gradually. Flu hits like a truck, usually within 12 to 24 hours of exposure.
A few things are worth watching when you suspect a second flu infection:
- Fever that spikes above 103°F, especially in adults, warrants a call to your doctor within 24 hours
- Shortness of breath or chest tightness indicates possible progression to pneumonia — seek care immediately
- Confusion or altered mental status in elderly patients is a medical emergency, not just a flu symptom
- Symptoms that improve and then worsen sharply after day 5 or 6 may indicate a secondary bacterial infection
This last point is critical. Secondary bacterial pneumonia following influenza is responsible for a significant portion of flu-related deaths. The virus damages the respiratory epithelium, creating an open doorway for Streptococcus pneumoniae, Staphylococcus aureus, and Haemophilus influenzae. A flu that seems to get better, then dramatically worse, is a red flag that warrants immediate evaluation.
How Long Are You Contagious After the Flu — and Does It Affect Others Getting It?
Most adults are contagious from one day before symptoms appear through five to seven days after symptoms begin. Children can be contagious for up to 10 days. Immunocompromised individuals may shed virus for weeks, sometimes without even feeling sick.
This has a direct bearing on back-to-back flu in households. If you recover from influenza A and your child brings home influenza B two weeks later, you are both susceptible and still in the recovery window. The chain of transmission within families is one of the most common mechanisms for back-to-back cases.
I know a family in Chicago — two parents, three school-age kids — who cycled through two different flu strains over eight weeks one winter. The parents got hit twice each. The kids, who had all received the flu vaccine that year, had milder second illnesses. Coincidence? Probably not.
Antiviral Medications and Back-to-Back Flu: What Actually Works
Antivirals are most effective when started within 48 hours of symptom onset — and they matter even more for a second flu infection. The three main options in the US as of 2025:
- Oseltamivir (Tamiflu): Oral pill, 75mg twice daily for 5 days. Reduces illness duration by 1–2 days and cuts complication risk. Generic versions are widely available; expect to pay $30–$50 with most insurance.
- Baloxavir marboxil (Xofluza): Single oral dose. Approved for ages 5 and up. More convenient, similar efficacy to Tamiflu, but costs more ($150–$200 without insurance). Good option when adherence to a 5-day course is a concern.
- Zanamivir (Relenza): Inhaled powder, twice daily for 5 days. Not appropriate for people with asthma or COPD. Less commonly prescribed but effective.
My strong recommendation: if you’ve already had the flu once in a season and you develop symptoms again, call your doctor the same day. Don’t wait to see if it gets better. The 48-hour window closes fast, and starting antivirals even one day late meaningfully reduces their effectiveness. Most telehealth platforms — including Teladoc, MDLive, and Amazon Clinic — can prescribe antivirals within hours.
Natural Immune Boosters: What Science Actually Supports
I’m going to be honest with you here: most “immune boosters” you’ll find in the supplement aisle are not supported by strong evidence for preventing flu. Some have modest data behind them. Others are pure marketing. Let me break down the honest state of the science.
Vitamin D: The best-supported supplement for respiratory infection prevention. A 2017 meta-analysis in BMJ covering 11,321 participants found that vitamin D supplementation reduced the risk of acute respiratory infection, with the strongest benefit in those who were deficient. If your vitamin D levels are low — which is common in northern latitudes in winter — supplementing with 1,000–2,000 IU daily is reasonable. This is not a flu cure. It’s a modest protective factor.
Zinc: Has shown some evidence for reducing the duration of cold symptoms when taken within 24 hours of onset. Evidence for influenza specifically is weaker. I wouldn’t rely on it, but it’s unlikely to harm you at standard doses (less than 40mg daily).
Elderberry (Sambucus): Popular, but evidence is mixed. A 2016 study in Nutrients showed reduced cold duration in air travelers. For flu specifically, a 2020 Cochrane-style review found insufficient evidence to draw firm conclusions. I’d categorize it as “worth trying, don’t count on it.”
Sleep: This is the one “supplement” with genuinely strong evidence. A landmark 2015 study in Sleep found that people who slept fewer than six hours per night were four times more likely to get a cold than those who slept seven or more hours. The data on flu is less direct, but immune memory consolidation during sleep is well-established. Seven to nine hours per night is not optional if you want your immune system performing at full capacity during recovery.
How to Protect Yourself After the First Flu — Practical Steps That Actually Work
The recovery window is when you’re most vulnerable, and it’s when most people do the least to protect themselves. Here’s what I’d tell anyone who has just recovered from the flu and wants to avoid going through it again.
- Stay home longer than you think you need to. The CDC recommends staying home until you’ve been fever-free for 24 hours without fever-reducing medication. I’d extend this to 48 hours, and I’d recommend wearing a mask in public settings for the first week back.
- Avoid crowded indoor spaces during the vulnerability window. Concerts, crowded gyms, packed restaurants — the two weeks after flu recovery are not the time. This is not about fear. It’s about biology. Your first-line defenses are down.
- Prioritize sleep aggressively. Your immune system does its most important repair work during deep sleep. Eight to nine hours during the recovery period isn’t indulgence. It’s medicine.
- Wash hands with soap and water for 20 seconds — religiously. Hand sanitizer is fine as a backup. Soap and water are better. This sounds basic because it is basic. It also works.
- Get the flu shot if you haven’t already. Even mid-season vaccination provides meaningful protection against strains you haven’t been exposed to yet. Talk to your doctor about timing if you’re still in active recovery.
- Consider N95 masking during peak flu weeks. I know mask fatigue is real. I also know N95 masks, when worn correctly, are highly effective at blocking respiratory droplets. In a year when both influenza A and B are co-circulating heavily, masking on public transit and in healthcare settings during your recovery window is not overcautious.
One thing I wish I’d known years ago: the flu doesn’t read your calendar. Taking three extra sick days when you feel 80% recovered isn’t a weakness. It’s a strategy.
Frequently Asked Questions About Getting the Flu Back to Back
Can you get the flu twice in one month?
Yes. If you were infected with influenza A in the first week of the month and exposed to influenza B in week three, you could be sick again by week four. This is uncommon but not rare in dual-strain seasons. Your immune system is particularly susceptible in weeks two through four following a flu infection. The more crowded your living or working environment, the higher the risk.
Is the second flu worse than the first?
It can be. A second flu during the recovery window — while your immune system is still rebuilding — often produces more severe symptoms and carries a higher risk of complications, including secondary bacterial pneumonia. Adults 65 and older, people with lung disease, and those who are immunocompromised face the greatest risk of serious illness with a second infection.
Do you have immunity after getting the flu?
You develop strain-specific immunity. If you had influenza A (H3N2), your antibodies are highly effective against that strain for several years. They offer minimal protection against influenza B or a different influenza A subtype. This is the core reason back-to-back flu is possible — the viruses are different enough that your immune system treats each one as a new threat.
How do I know if I have the flu or just a cold the second time?
The classic flu indicators are sudden onset (symptoms develop quickly over hours, not days), high fever above 101°F, severe muscle aches, profound fatigue that keeps you bedridden, and a dry, persistent cough. Colds typically begin with a sore throat and runny nose, develop gradually, and produce a milder fever. At-home rapid flu tests available at pharmacies can confirm influenza within 15 minutes. Test as early as possible for the most accurate results.
Can I get the flu from someone who is vaccinated?
Yes, though the vaccinated person is less likely to be contagious and less likely to shed the virus for as long. Vaccinated individuals who do catch the flu tend to have shorter, milder illnesses, which means reduced virus shedding. They’re not zero risk, but they’re lower risk. This is one of the public health arguments for broad vaccination coverage: protecting not just the individual but also reducing overall community transmission.
Should I get another flu shot if I’ve already had the flu this season?
Talk to your doctor. Generally, if you’ve already had the flu and recovered, and you were vaccinated before the season, an additional shot isn’t recommended or available. If you had the flu but weren’t vaccinated, getting the flu shot can still protect you against other circulating strains. Timing matters here: most doctors recommend waiting at least two weeks after recovery before vaccinating.
What is the fastest way to recover from back-to-back flu?
Start antiviral treatment within 48 hours if your doctor agrees. Prioritize sleep above everything else. Stay hydrated with water, broth, and electrolyte drinks. Avoid alcohol and caffeine in excess, both of which impair immune function and sleep quality. Eat protein-rich foods to support immune cell production. And genuinely rest — not Netflix-in-bed rest, but actual sleep. The more aggressively you recover, the shorter your vulnerability window for a third illness.
The Bottom Line on Back-to-Back Flu
Back-to-back flu is not bad luck. It’s biology. Influenza is a diverse, fast-evolving family of viruses that doesn’t reward past suffering with future immunity. Different strains circulate simultaneously, your immune system is temporarily vulnerable after the first infection, and most people return to high-exposure environments long before their defenses are fully rebuilt.
Sarah, my neighbor, went through eight weeks of misery because she didn’t know her recovery window was a vulnerability window. She knows now. She was vaccinated the following October, took an extra four days off after her next respiratory illness, and used the telehealth option to get antivirals at the first sign of symptoms. She made it through the next flu season without a second illness.
The flu is beatable — not by ignoring the biology, but by understanding it. Get vaccinated every year. Treat symptoms early. Protect your recovery window like the critical period it actually is. And if you do get hit twice, know that you are not uniquely unlucky. You’re dealing with a virus that is specifically designed to be elusive.
What’s your experience with back-to-back illness during flu season? Have you found specific strategies that helped your recovery? I’d genuinely like to know — the patterns people notice in their own bodies often reveal things the research hasn’t caught up to yet.